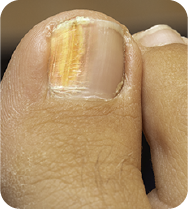
Onychomycosis typically presents as a progressive infection of the nail unit. Pharmacists should be adept at recognizing the clinical subtypes, most commonly Distal Lateral Subungual Onychomycosis (DLSO).
Early Manifestation:
- Leukonychia: Often presents initially as white or yellow opacities in the nail plate (specifically in White Superficial Onychomycosis or early DLSO).
Progressive Pathology:
- Chromonychia: Discoloration ranging from yellow/white to brown.
- Subungual Hyperkeratosis: Accumulation of debris under the nail plate leading to thickening (onychauxis).
- Onycholysis: Detachment of the nail plate from the nail bed.
- Dystrophy: Crumbling, splitting, or total destruction of the nail plate.
- Odor: Malodorous debris may be present due to secondary bacterial colonization or fungal metabolic byproducts.
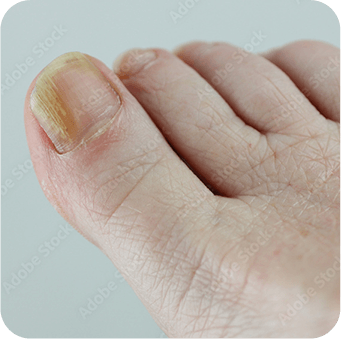
Etiology and Pathogenesis
Onychomycosis is a fungal infection of the nail apparatus (matrix, bed, or plate). Pathogens generally invade the hyponychium or lateral nail folds.
Pathogenic Profile:
- Dermatophytes: Account for approximately 90% of toenail infections.
- Trichophyton rubrum is the primary pathogen.1
- Trichophyton mentagrophytes is the second most common
- Non-Dermatophyte Molds (NDMs) & Yeasts:
- Candida species (more common in fingernail infections or chronic
- NDMs such as Scopulariopsis, Fusarium, and Aspergillus species are causative in a minority of cases but may be resistant to standard therapies 1.
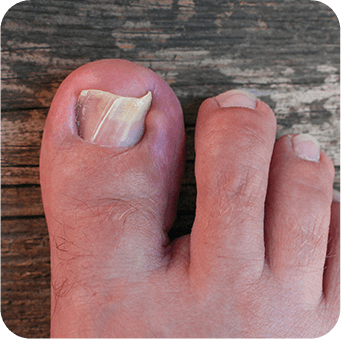
Risk Stratification & Patient History
While prevalence increases with age, specific comorbidities significantly elevate risk.
- Trauma: Prior history of micro- or macro-trauma to the nail unit creates portals of entry.
- Immunosuppression: HIV, chemotherapy, or chronic corticosteroid use.
- Diabetes Mellitus: Patients with diabetes are at significantly higher risk due to neuropathic and vascular changes. Studies indicate that approximately one-third of diabetic patients suffer from onychomycosis.2
- Concurrent Tinea Pedis: A major predictor; the presence of Tinea pedis is strongly associated with the development of onychomycosis due to the spread of the same dermatophyte.3
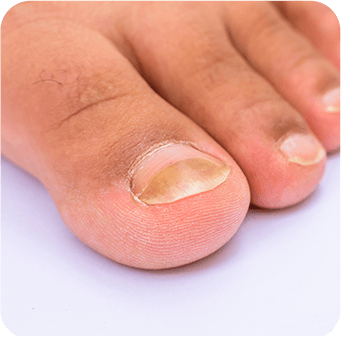

Clinical Red Flag:
The Diabetic Patient
In diabetic patients, onychomycosis is not merely cosmetic; it is a risk factor for foot ulceration, cellulitis, and gangrene. Pharmacists should refer diabetic patients presenting with onychomycosis for professional podiatric or medical assessment to rule out secondary bacterial infection and assess vascular status.2
References
1 Piraccini BM, Alessandrini A. (2015). Onychomycosis: A Review. Journal of Fungi, 1(1), 30-43.
2 Loo, D. S. (2007). Onychomycosis in the elderly: drug treatment options. Clinical Interventions in Aging, 2(2), 285–292.
3 Rosen, T., et al. «Management of Onychomycosis and Co-Existing Tinea Pedis.» Journal of Drugs in Dermatology 14.7 (2015): s35-s39.