Corns and calluses in pharmacy practice: recognition and risk assessment
Corns and calluses are common foot lesions caused by repeated pressure or friction. Although benign, they frequently lead patients to seek advice in community pharmacy due to discomfort, pain, or difficulty walking.
Pharmacists play an important role in recognising these conditions, identifying contributing factors, and ensuring timely referral when needed.
What are corns and calluses?
Corns and calluses are areas of localised thickening of the skin (hyperkeratosis) that develop as a protective response to repeated mechanical stress 1, 2.
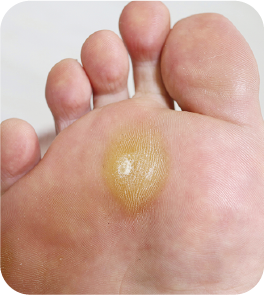
Corns are small, well-defined areas of hard skin that typically form over bony prominences and may cause sharp, localised pain 3.
Calluses are broader, more diffuse areas of thickened skin, most often found on weight-bearing areas such as the heel or the ball of the foot.
Both result from ongoing pressure or friction rather than infection or inflammation 2, 4.
Common causes and contributing factors
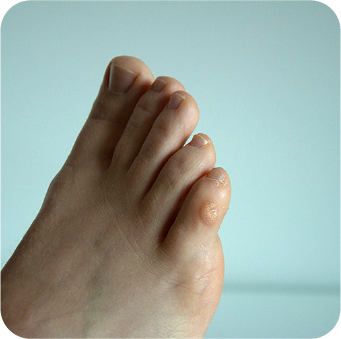
The most common cause of corns and calluses is repeated pressure from footwear. Tight, ill-fitting, or poorly cushioned shoes, including shoes with narrow toe boxes or high heels, increase friction and focal pressure on the foot.
Underlying foot deformities, such as hammer toe, claw toe, or hallux valgus, further increase pressure on specific areas and are associated with recurrent lesions 2, 4, 5.
Clinical presentation in pharmacy
Patients may report:
- Localised pain or tenderness when walking or standing
- A burning or aching sensation after prolonged activity
- Difficulty wearing certain footwear
On inspection, corns appear as small, centralised areas of hard skin, while calluses present as thicker, diffuse plaques of hyperkeratosis.
Corns and calluses are more frequently observed in older adults, reflecting age-related changes in skin elasticity, fat padding, and gait mechanics6.
Impact on daily function
Although not dangerous in themselves, corns and calluses can significantly affect comfort, mobility, and gait. Pain may lead patients to alter how they walk, potentially increasing the risk of secondary problems such as joint strain, imbalance, or skin breakdown, particularly in older adults or those who stand for long periods 3.
Identifying patients at increased risk
Most corns and calluses can be managed conservatively. However, pharmacists should be alert to higher-risk patients, particularly those with:
- Diabetes mellitus
- Peripheral vascular disease
- Reduced sensation or neuropathy
- Compromised immune function
In these individuals, even minor skin lesions can progress to ulceration or infection and require medical or podiatric assessment 7-9
When to refer
Referral to a GP or podiatrist is recommended when:
- Corns or calluses are large, painful, or recurrent
- Symptoms persist despite appropriate self-care
- There is diagnostic uncertainty
- The patient has diabetes, vascular disease, or reduced sensation
Early referral helps prevent complications and supports safe management.
Resources
- Al Aboud, A.M. and S.N.S. Yarrarapu, Corns, in StatPearls. 2025: Treasure Island (FL) ineligible companies. Disclosure: Siva Naga Yarrarapu declares no relevant financial relationships with ineligible companies.
- Freeman, D.B., Corns and calluses resulting from mechanical hyperkeratosis. Am Fam Physician, 2002. 65(11): p. 2277-80.
- Demir, B., et al., Quality of life in patients with calluses. Int J Dermatol, 2016. 55(1): p. e47-9.
- Singh, D., G. Bentley, and S.G. Trevino, Callosities, corns, and calluses. BMJ, 1996. 312(7043): p. 1403-6.
- Abu-Qamar, M.Z., et al., Foot Problems in Patients in Acute Care: A Point-Prevalence Survey. J Wound Ostomy Continence Nurs, 2020. 47(5): p. 513-520.
- Ricci, V., A.J. Abdulsalam, and L. Ozcakar, From Plantar Fasciitis to Heel Fat Pad Syndrome: Sonographic Kaleidoscope for Heel Pain. Am J Phys Med Rehabil, 2024. 103(11): p. e172-e173.
- Armstrong, D.G., A.J.M. Boulton, and S.A. Bus, Diabetic Foot Ulcers and Their Recurrence. N Engl J Med, 2017. 376(24): p. 2367-2375.
- Bus, S.A., et al., Guidelines on the prevention of foot ulcers in persons with diabetes (IWGDF 2023 update). Diabetes Metab Res Rev, 2024. 40(3): p. e3651.
- Zanni, G.R. and J.Y. Wick, Delving into foot mechanics and related problems. Consult Pharm, 2011. 26(12): p. 890-901.






