Verrucas and common warts in pharmacy practice: recognition and risk assessment
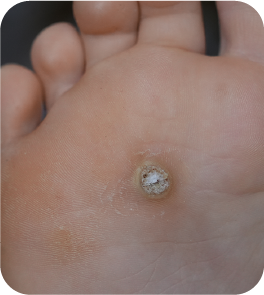
Verrucas are plantar warts caused by infection with the human papillomavirus (HPV). They develop on the soles of the feet or toes, typically in weight-bearing areas exposed to pressure or friction 1,2.
In community pharmacy, patients may seek advice due to discomfort, uncertainty about the diagnosis, or concerns about persistence and spread.
Recognizing verrucas
Typical features include:
- A rough or grainy surface
- Interruption of normal skin lines
- Small dark dots representing thrombosed capillaries
- Discomfort or pain on weight-bearing, sometimes described as “walking on a pebble” by the patient
Because of their location, verrucas may interfere with walking and daily activities, prompting patients to seek advice early.
Understanding common warts
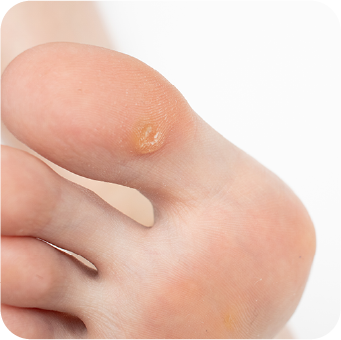
Common warts are hyperkeratotic skin growths that usually occur on the hands, fingers, or other non-weight-bearing areas 1.
They typically:
- Are skin-colored or slightly grey
- Have a rough, cauliflower-like surface
- Measure a few millimeters in diameter
Although medically benign, common warts may cause cosmetic concern or anxiety about transmission, particularly when lesions are visible or multiple.
Natural course of verrucas and warts
How infection spreads
HPV thrives in environments that promote skin maceration and microtrauma 1, 5.
Transmission is more likely through:
- Barefoot exposure in communal areas such as swimming pools and changing rooms
- Shared towels, footwear, or contaminated surfaces
- Autoinoculation from scratching or shaving affected areas
The presence of broken or softened skin increases susceptibility to infection.
Patients at increased risk
Anyone can develop verrucas or common warts; however, they are more frequently observed in 1, 5:
- Children and adolescents
- Individuals who frequently walk barefoot in communal environments
- People with reduced immune function
In immunocompromised patients, lesions may be more extensive, persistent, or atypical and warrant closer assessment 6.
When to consider referral
Referral to a general practitioner or dermatologist may be appropriate when:
- The diagnosis is uncertain
- Lesions are extensive, persistent, or refractory
- The patient is immunocompromised
- There is significant pain or functional impairment
Early identification of higher-risk patients supports appropriate onward care.

The pharmacist’s role
Pharmacists play an important role in recognising the characteristic symptom pattern of plantar fasciitis, reassuring patients about the nature of the condition, and guiding them toward appropriate next steps, including conservative care and referral when needed.
💡 Clinical distinction: verrucas vs common warts
Verrucas and common warts are caused by the same virus (HPV). The key clinical difference lies in their location and associated symptoms. Verrucas develop on weight-bearing areas of the foot and may cause pain on walking, whereas common warts typically occur on the hands and are rarely painful.
Resources
- Witchey, D.J., et al., Plantar Warts: Epidemiology, Pathophysiology, and Clinical Management. J Am Osteopath Assoc, 2018. 118(2): p. 92-105.
- Garcia-Oreja, S., et al., Topical treatment for plantar warts: A systematic review. Dermatol Ther, 2021. 34(1): p. e14621.
- Bruggink, S.C., et al., Natural course of cutaneous warts among primary schoolchildren: a prospective cohort study. Ann Fam Med, 2013. 11(5): p. 437-41.
- Kwok, C.S., et al., Topical treatments for cutaneous warts. Cochrane Database Syst Rev, 2012. 2012(9): p. CD001781.
- Sterling, J.C., et al., British Association of Dermatologists’ guidelines for the management of cutaneous warts 2014. Br J Dermatol, 2014. 171(4): p. 696-712.
- D’Souza, G.F. and J.E. Zins, Severe Plantar Warts in an Immunocompromised Patient. N Engl J Med, 2017. 377(3): p. 267.






