The pharmacist’s role in wart and verruca management
Warts and verrucas are common, usually benign skin lesions encountered in pharmacy practice.
Pharmacists play a central role in their management through education, expectation management, and evidence-based treatment selection. Equally important is recognizing when specialist assessment is required and ensuring timely referral when appropriate.
Understanding warts and verrucas
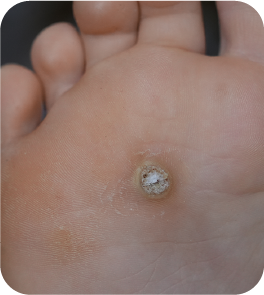
Cutaneous warts are caused by infection with the human papillomavirus (HPV). Common warts (verruca vulgaris) typically affect the hands and fingers, while plantar warts develop on the soles of the feet, often at pressure points. Verrucas may be painful when walking and can usually be distinguished from calluses by interruption of normal skin lines and the presence of small thrombosed capillaries (“black dots”) 1, 2.
Warts may clear without treatment, but studies in primary care populations show that resolution can take many months or longer, particularly in children and adolescents 3. After infection with HPV, warts may also take several months to appear. The likelihood of contracting the virus can be increased by microtrauma to the skin, which facilitates viral entry. As a result, many patients seek advice or treatment to relieve discomfort and limit spread.
First-line management in pharmacy
From a pharmacy perspective, management should begin with reassurance and a discussion of available treatment options, taking into account symptoms, patient preference, and safety. For asymptomatic or mildly symptomatic warts, active monitoring may be appropriate, alongside advice on hygiene and self-care.
When treatment is requested, several over-the-counter options are available in pharmacy practice. These include topical acid-based treatments (e.g., salicylic acid or trichloroacetic acid preparations), which exert a keratolytic effect and progressively remove hyperkeratotic tissue, as well as cryotherapy products, which induce local tissue destruction through rapid freezing. These treatments are available in a range of formulations, including solutions, gels and medicated plasters 4, 5.
Pharmacists should emphasize the importance of regular application (often daily), protecting surrounding healthy skin, and maintaining treatment for several weeks to months. Adherence is critical, as inconsistent use significantly reduces effectiveness.
Over-the-counter cryotherapy can also be considered in pharmacy practice. Treatment response may vary, and pharmacists should advise that repeated applications are often required 5, 6.
Simple measures, such as gently removing thickened skin before treatment and advising patients not to pick or shave lesions, may help reduce spread and improve treatment effectiveness.
When not to treat and when to refer
L’HPV si sviluppa più facilmente in ambienti che favoriscono macerazione cutanea e microtraumi della pelle1,5.
La trasmissione avviene più frequentemente tramite:
- esposizione a piedi nudi in aree condivise, come piscine o spogliatoi
- condivisione di asciugamani, calzature o superfici contaminate
- autoinoculazione, dovuta a manipolazione, grattamento o rasatura
La presenza di pelle danneggiata o ammorbidita aumenta il rischio di infezione.
Fattori di rischio
- The diagnosis is uncertain (e.g., pigmented, bleeding, or rapidly changing lesions)
- Warts are painful, infected, or extensive
- The patient is immunocompromised
- Lesions persist despite several months of appropriate treatment
- Painful plantar warts that significantly impair walking may benefit from referral to a general practitioner or podiatrist for further assessment and management.
💡DID YOU KNOW?
People often confuse plantar warts and calluses. Help your patients tell the difference:
| Plantar wart | Callus |
Cause | Viral (HPV) | Repeated pressure or friction |
Surface | Rough or irregular | Smooth, thickened skin |
Black dots | May be present | Absent |
Pain | Often painful when walking or when squeezed | More painful with direct pressure |
Management | Observation or targeted treatment | Pressure relief and skin care |
- Sterling, J.C., et al., British Association of Dermatologists’ guidelines for the management of cutaneous warts 2014. Br J Dermatol, 2014. 171(4): p. 696-712.
- Witchey, D.J., et al., Plantar Warts: Epidemiology, Pathophysiology, and Clinical Management. J Am Osteopath Assoc, 2018. 118(2): p. 92-105.
- Bruggink, S.C., et al., Natural course of cutaneous warts among primary schoolchildren: a prospective cohort study. Ann Fam Med, 2013. 11(5): p. 437-41.
- Kwok, C.S., et al., Topical treatments for cutaneous warts. Cochrane Database Syst Rev, 2012. 2012(9): p. CD001781.
- Garcia-Oreja, S., et al., Topical treatment for plantar warts: A systematic review. Dermatol Ther, 2021. 34(1): p. e14621.
- Garcia-Oreja, S., et al., Efficacy of cryotherapy for plantar warts: A systematic review and meta-analysis. Dermatol Ther, 2022. 35(6): p. e15480.
- D’Souza, G.F. and J.E. Zins, Severe Plantar Warts in an Immunocompromised Patient. N Engl J Med, 2017. 377(3): p. 267.